What is Sciatica
Did you know that the sciatic nerve is the longest nerve in your body? It runs from your lower back, through your glutes, and down the back of each leg. No wonder it causes so many long lingering problems. This long nerve controls many of the muscles and sensations in your legs. After hip resurfacing surgery, sometimes, although rarely, this nerve can get irritated. SciaticaIf you are experiencing a lot of pain post op, more than the average person, then read the symptoms below and hopefully these articles will help.
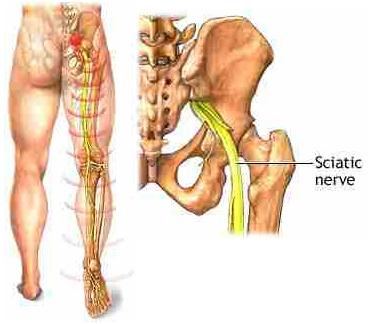 Sciatica refers to the pain you feel along this nerve. It can be described as shooting pain, tingling, burning, numbness, or weakness that travels from your lower back down the back of your leg. If you have had issues with your sciatic nerve you will know what I am talking about. Sciatica pain isn't a disorder, but rather a symptom of a larger problem, usually a bulging or herniated vertebral disk. This is the most common cause of sciatica nerve pain, but other spinal issues such as a tumor (yikes!) or injury (major hip surgery) could also be the cause. A condition called *Piriformis syndrome, can also cause sciatica. This is when the piriformis muscle tightens spasms, putting pressure on the nerve creating pain. Active women like runners and serious walkers, and people who sit for long periods of time are especially likely to develop this condition.
Sciatica refers to the pain you feel along this nerve. It can be described as shooting pain, tingling, burning, numbness, or weakness that travels from your lower back down the back of your leg. If you have had issues with your sciatic nerve you will know what I am talking about. Sciatica pain isn't a disorder, but rather a symptom of a larger problem, usually a bulging or herniated vertebral disk. This is the most common cause of sciatica nerve pain, but other spinal issues such as a tumor (yikes!) or injury (major hip surgery) could also be the cause. A condition called *Piriformis syndrome, can also cause sciatica. This is when the piriformis muscle tightens spasms, putting pressure on the nerve creating pain. Active women like runners and serious walkers, and people who sit for long periods of time are especially likely to develop this condition.
How can you treat sciatica?
- Cold packs can help alleviate some of the pain in the first 2 hours by relieving inflammation.
- After experiencing symptoms for 48 hours, applying heat packs to the painful areas is recommended. If you still feel discomfort, alternate between cold and hot packs.
- Gentle stretching for your lower back may also help relieve nerve pressure.
- If you have moderate pain, over the counter meds may help.
- If your pain is more severe, prescriptions drugs may relieve pain more effectively.
- Physical therapy or Pilates exercises to correct your posture and strengthen your back and core muscles can also help in your recovery.
- Massage therapy may also help relieve tightness in muscles, which can cause sciatica pain.
- Going to a chiropractor may also help to improve your posture and spinal alignment.
- Regular exercise is still important to help combat chronic discomfort. It release endorphins, which are chemicals that prevent pain signals from reaching your brain.
- Depending on your condition, your doctor may also use corticosteroid injections to help relieve inflammation.
- If your sciatica is very severe, and causes extreme weakness in the lower legs, and loss of bowel control, surgery may be recommended to remove part of the herniated disk.
You should definitely talk to your doctor about what may be causing your sciatica so you can get the necessary treatment.
Another explanation of Sciatica
Sciatica is a set of symptoms including pain that may be caused by general compression and/or irritation of one of five nerve roots that give rise to the sciatic nerve, or by compression or irritation of the sciatic nerve itself. The pain is felt in the lower back, buttock, and/or various parts of the leg and foot. In addition to pain, which is sometimes severe, there may be numbness, muscular weakness, and difficulty in moving or controlling the leg. Typically, the symptoms are only felt on one side of the body. Although sciatica is a relatively common form of low back pain and leg pain, the true meaning of the term is often misunderstood. Sciatica is a set of symptoms rather than a diagnosis for what is irritating the root of the nerve, causing the pain. This point is important, because treatment for sciatica or sciatic symptoms will often be different, depending upon the underlying cause of the symptoms.Although sciatica is common, a 2008 review of clinical trials said there are no good treatments for it. "Pain Treatment for Sciatica - Full Text View - ClinicalTrials.gov The first cited use of the word "sciatica" was registered in 1450.
Causes of sciatica
Sciatica is generally caused by the compression of lumbar nerves L4 or L5 or scral nerves scS1, S2 or S3, or far less commonly, by compression of the sciatic nerve itself. When sciatica is caused by compression of a dorsal nerve root (radix) it is considered a lumbar radiculopathy (or radiculitis when accompanied with an inflammatory response) from a spinal disc herniation (a herniatedintervertebral disc in the spine), or from roughening, enlarging, and/or misaligning of the vertebrae (spondylolisthesis), or degenerated discs. Sciatica due to compression of a nerve root is one of the most common forms of radiculopathy. "Pseudo-sciatica," which causes symptoms similar to spinal nerve root compression, is caused by the compression of peripheral sections of the nerve, usually from soft tissue tension in the piriformis or related muscles (see piriformis syndrome below).
Spinal disc herniation
One cause of sciatica is a spinal disc herniateion, pressing on one of the sciatic nerve roots. The spinal discs are composed of a tough spongiform ring of cartilage (annulus fibrosus) with a more malleable center (nucleus pulposis). The discs separate the vertebrae, thereby allowing room for the nerve roots to properly exit through the spaces between the L4, L5, and sacral vertebrae. The discs cushion the spine from compressive forces, but are weak to pressure applied during rotational movements. That is why a person who bends to one side, at a bad angle to pick something up, may more likely herniate a spinal disc than a person falling from a ladder and landing on his or her back. Herniation of a disc occurs when the liquid center of the disc bulges outwards, tearing the external ring of fibers, extrudes into the spinal canal, and compresses a nerve root against the lamina or pedicle of a vertebra, thus causing sciatica. This extruded liquid from the nucleus pulposus may cause inflammation and swelling of surrounding tissue which may cause further compression of the nerve root in the confined space in the spinal canal. Sciatica caused by pressure from a disc herniation and swelling of surrounding tissue can spontaneously subside if the tear in the disc heals and pulposis extrusion and inflammation cease. Sciatica can be caused by tumours impinging on the spinal cord or the nerve roots. Severe back pain extending to the hips and feet, loss of bladder or bowel control, or muscle weakness, may result from spinal tumours. Trauma to the spine, such as from a car accident, may also lead to sciatica.
Spinal stenosis
Other compressive spinal causes include spinal stenosis, a condition wherein the spinal canal (the spaces through which the spinal cord runs) narrows and compresses the spinal cord, cauda equina, and/or sciatic nerve roots. This narrowing can be caused by bone spurs, vertebral dislocation, inflammation, or herniated disc which decreases available space for the spinal cord, thus pinching nerves from the spinal cord that travel to the sciatic nerve and irritating them with friction.
Piriformis syndrome
In 15% of the population, the sciatic nerve runs through the piriformis muscles rather than beneath it. When the muscle shortens or spasms due to trauma, it can compress or strangle the sciatic nerve beneath the muscle. This cause of sciatic symptoms is piriformis syndrome. This may be the major cause of sciatica when the nerve root is normal.
Trigger points
Another source of sciatic symptoms is active trigger points of the lower back and the gluteus muscles. In this case, the referred pain is not consequent to compression of the sciatic nerve, though the pain distribution down the buttocks and leg is similar. Trigger points occur when muscles become ischemic (having low blood flow) due to injury or chronic muscular contraction. The most commonly associated muscles with trigger points triggering sciatic symptoms are: the quadratus lumborum, the gluteus medius, the gluteus minumus, and the deep hip rotators.
Habits
The risk of self-inflicted sciatica has increased in recent years with the fashion trend of lower-hanging trousers as well as lower-positioning of the pockets. For instance, sitting on a wallet for prolonged hours every day can cause self-inflicted sciatica. Symptoms of numbness and/or pain behind the knee cap are associated with this form of sciatica. Work-related sciatica may be caused by the use of tool belts by carpenters which hang around the hips and cause significant misalignment of the sacral vertebrates over long time periods.
Diagnosis and treatment
Because of the many conditions which can compress nerve roots and cause sciatica, treatment and symptoms often differ from patient to patient. Diagnostic tests can come in the form of a series of exams a physician will perform. Patients will be asked to adopt numerous positions and actions such as squatting, walking on toes, bending forward and backward, rotating the spine, sitting, lying on back, and raising one leg at a time. Increased pain will occur during some of these activities. Treatment of the underlying cause of the compression is often the most effective course. When the cause is due to a prolapsed or lumbar disc herniation, research has shown that, with supportive treatment to help relieve pain, 90% of disc prolapse will recover with no specific intervention. Genetics appear to influence the risk of developing disc herniation. Imaging methods such as MR neurography may help diagnosis and treatment of sciatica. MR neurography has been shown to diagnose 95% of severe sciatica patients, while as few as 15% of sciatica sufferers in the general population are diagnosed with disc-related problems. MR neurography is a modified MRI technique using MRI software to provide better pictures of the spinal nerves and the effect of compression on these nerves. MR neurography may help diagnose piriformis syndrome which is another cause of sciatica that does not involve disc herniation. Most cases of sciatica can be treated by one or more of the following:
- Acupuncture
- Anti-inflammatory medications (e.g. NSAIDs or oral steroids though NSAIDs are no more effective than a placebo for acute sciatica.
- Chiropractic
- Osteopathy
- Non-surgical spinal decompression
- Physical therapy
- Surgery
- Stretching exercises
- Structural integration
Specific surgical techniques include:
Intradiscal Electrothermoplasty (IDET)
A needle is inserted into the affected disc, guided by X-ray. A wire is then threaded down through the needle and into the disc until it lies along the inner wall of the annulus. The wire is then heated which destroys the small nerve fibers that have grown into the cracks and have invaded the degenerating disc. The heat also partially melts the annulus, which triggers the body to generate new reinforcing proteins in the fibers of the annulus.
Radiofrequency Discal Nucleoplasty (Coblation Nucleoplasty)
A needle is inserted into the affected disc, although instead of a heating wire, a special RF probe (radio frequency) is used. This probe generates a highly focused plasma field with enough energy to break up the molecular bonds of the gel in the nucleus, essentially vaporizing some of the nucleus. The result is that 10-20% of the nucleus is removed which decompresses the disc and reduces the pressure both on the disc and the surrounding nerve roots. This technique may be more beneficial for sciatica type of pain than the IDET, since nucleoplasty can actually reduce the disc bulge, which is pressing on a nerve root. The high-energy plasma field is actually generated at relatively low temperatures, so danger to surrounding tissues is minimized.
Piriformis syndrome. Running directly above the sciatic nerve, the piriformis muscle starts at your lower spine and connects to each thighbone (femur). Piriformis syndrome occurs when the muscle becomes tight or goes into spasms, putting pressure on the sciatic nerve. The pain may radiate down the back of your thigh but doesn't extend below the knee. Prolonged sitting, car accidents and falls also can contribute to piriformis syndrome.
